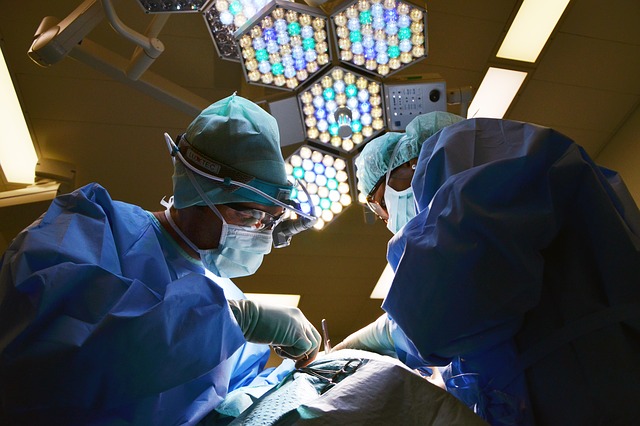
A new study has found that fatigue does not affect a surgeon’s performance. Researchers from the University of Toronto say that lack of sleep from the night before will not make surgeons more likely to make mistakes.
The results showed that patients had a 22.2 percent (22.2%) chance of experiencing a surgery-related issue when their surgeon had spend the nigh before (the 12 am to 7 am work shift) treating patients, and 22.4 percent (22.4%) chance of experiencing a surgery-related issue when their surgeon had spend the nigh before resting.
Dr. Nancy Baxter, senior author on the study and surgery division chief from St. Michael’s Hospital (Toronto), gave a statement saying that “I believe what we are seeing in our study reflects self-regulation — that surgeons plan around their schedules based on their individual ability to tolerate sleep deprivation. Given our findings, they seem to be doing a good job of it”.
For their study, Dr. Baxter and her team looked at about 39.000 patients who were undergoing one of the 12 daytime surgeries examined in the study, and at 1.400 surgeons.
The researchers paired each patient with another individual who had the same procedure performed by the same surgeon. One of the patients got the surgeon after a good night’s sleep, and the other got him or her right after they worked a night shift.
The researcher team surveyed each patient for 30 days after they had their operation and concluded that patients who got the surgeon after a good night’s sleep did not experience a different outcome than those who got the same surgeon after working the whole night.
However the study is not without controversy as Dr. Carlos Pellegrini, American College of Surgeons past president and current chair of surgery from the University of Washington Medicine (Seattle), gave a statement of his own saying that these findings trouble him.
He admitted that the study is very polished and does not seem to be misleading the public, but he also added that he is concern that people who have been hounding the belief that surgeons can spend the entire night operating and then keep operating in the morning, don’t think that this paper confirms that surgeons can do that and still have the same outcomes.
Dr. Baxter agrees with Dr. Pellegrini. She said that if hospitals were to take away a physician’s ability to self-regulate their work when being on call after working the night before, “the potential to cause harm” would be very real.
She went on to add that sleep deprivation affects all of us, it’s just that some people can deal with it well, while other deal with it poorly, and the only person who can judge how a specific physician deals with it is the physician himself / herself.
She pointed out that the main discovery she and her team made is that physicians are generally very good at judging this for themselves, and take the appropriate steps to modifying their practice accordingly.
Dr. Baxter also informed that the Sleep Research Society requires surgeons who’ve been awake for at least 22 hours straight to tell their patients about their sleep deprivation and ask them whether they feel comfortable with the circumstances or if they’d like to request another surgeon.
The findings were published earlier this week, on Wednesday (August 26, 2015), in the New England Journal of Medicine.
Image Source: pixabay.com

Leave a Reply
You must be logged in to post a comment.